Have we got lots to learn from the Dutch? Natalie's reflection
/Hello!
Sheena asked me to write a little bit about my experience of my midwifery elective placement in The Hague, the Netherlands. This was a very exciting however, I have never written for a blog before and hope it is interesting enough to read! So here we go:
My name is Natalie Buschman, and I have recently finished my midwifery degree at King’s College London. At the end of our third year we are given the opportunity to work in a different place or country for 2 weeks, and I arranged to go to the Netherlands. I am actually Dutch, but have lived in the UK for the last 17 years, and had my own two children here in the UK. I therefore have never experienced the Dutch maternity system and only know what the majority of birth workers know: the Netherlands is the envy of the world keeping birth physiological without unnecessary medical interventions. The Netherlands is well known for their high home birth rate and while this has steadily declined from 35% in 2000 to 16% in 2013 (Brouwers, Bruinse, Dijs-Elsinga et al., 2014) for a variety of reasons, it is still high in comparison with meagre 2.3% in the UK(Birth Choice UK, 2011), and certainly a desirable statistic to have! Furthermore a rather unique feature of Dutch maternity care is the “kraamverzorgster” who can be described as a maternity nurse or postnatal doula supporting families after they have a baby. A kraamverzorgster is available to all women and their families, regardless of income. They will assist the midwife during homebirth or in the hospital (midwife-led) during labour and are available for undivided postnatal care for the first week. All in all, my elective was a great opportunity to go home and have a taste of this highly acclaimed maternity care system.
Ellie the kraamverzorgster with traditional ‘beschuit met muisjes’ or crispbake with mice (aniseed with a sugar coating)
The first thing I quickly need to explain is the concept ‘first line’ and ‘second line’ midwifery care. In the Netherlands, like in the UK, you can self-refer to a midwife. Women will contact their midwife/midwifery practise of choice directly for low risk care; this is considered the first line. Only if there are any underlying medical conditions and/or any complications arise during the pregnancy, will the midwife refer the women through to the second line or obstetric care. As such there is a definite divide between first and second line care. As a newly qualified midwife in the Netherlands you are a first line midwife, unless you choose to work in the hospital under obstetric supervision as a second line midwife. Overall, as a second line midwife, you look after women who are already under obstetric care in their pregnancy or who become higher risk for any reason during their labour and birth OR for maternal request for pharmaceutical pain relief such as an epidural. As a first line midwife you look after all women without any specified risks. There is also third line care, which are the big academic specialist hospitals for which women need a referral from the second line or general hospitals.
Midwives Chantal, Anke, Peggy, Carola and Rachelle, their main interim midwife, from midwifery group practice “Anno” in the Hague welcomed me for two weeks this past August and indulged my curiosity. Anno is an established practice with, on average, between 30 and 35 women on their books each month.
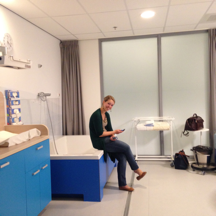
Light airy clinical room at Anno’s home base in the Tree and Flower quarter
It is usual for a midwifery practice to have a ‘shop front’ in the Netherlands, and Anno’s is warm and inviting with a nice airy waiting area and two welcoming clinical rooms located in the tree and flower quarter of The Hague. They offer preconception, antenatal and six week follow up appointments (if desired as most women do not do this) at Anno’s home base as well as an antenatal clinic at two different GP’s. The midwives will do home births or hospital births, whatever the women desire. Their homebirth rate of approximately 6.5% (about 2 births per month) and is much lower than the latest national average of 16%, which the midwives felt, is due to a ‘city’ thing as well as the population they serve. Additionally, Anno offers dating and growth scans. First line midwives, and hospitals, earn their income from the woman’s health insurance; therefore due to the high percentage of Dutch midwives working independently, competition is fierce. The idea that you can have your first scan done with your midwife is an appealing one. Perhaps this makes the difference in the amount of women who will go for their nuchal scan and combination test whether there are any chromosomal abnormalities, with the most commonly known being Down’s syndrome, in their pregnancy. Roughly 50% of the women booked at Anno will go for this test after being counselled by one of the midwives, while in my experience at the Trust where I trained, the vast majority of women will have this test done. It felt like there was a more conscious decision on what they would do with the information rather than going ‘along’: an opt-in instead of an opt-out.
Before I started, the midwives had requested a little ‘bio’ from me and a photograph so the women they cared for could read about me before meeting me. I thought this was a nice touch, and on several occasions the women’s reaction to me was “I was just reading about you - how fun you are from London!” The next comment was mostly how good my Dutch was! While it is my mother tongue, I have to admit that I mostly eat, sleep and dream English so switching back did cause some initial giggles all round with some literal translations and weird sentence constructions on my part! Luckily, the Dutch side of my brain kicked in fairly quickly and it even managed to get to grips with the Dutch midwifery dialect (i.e. jargon!). In order to get the most rounded experience in my very short time, I spent time in the antenatal clinic at Anno’s home base as well as at the GP surgery which serves a very large immigrant population, predominately Turkish and Moroccan women, scanning clinic, postnatal visits and being on call for anything and everything. I was also privileged to be at two births and while they were not at home, it was still a great opportunity to see the midwives in action and how it worked being in a hospital without working for that hospital!
So what are my thoughts after this whirlwind of Dutch maternity care? I can only really share my thoughts on the first line midwifery care, as this is what I observed. There were some practical things like how amazing it would be to have kraamverzorgsters, who take care of most of the clinical postnatal issues such as checking stitches, whether the uterus is well contracted, mum’s pulse etc. They also support the family in how to take care of the baby and of course give invaluable breastfeeding support. A midwife visits every other day for at least 8 days, checks with the kraamverzorgster if there are any concerns and there is actually an opportunity to ask the woman how she is! Don’t get me wrong, there was not necessarily time for a cuppa but it definitely felt less rushed then what I have experienced in the UK. Something that did stand out for me was the amount of women that were expressing breast milk. I just did not understand why they expressed rather than put the baby on the breast? What I did forget is that though the Netherlands has an excellent maternity care package, it is very short! Women in the Netherlands are entitled to 16 weeks paid leave (at 100% pay), and are expected to start their maternity leave at minimum 4 weeks before their baby is due. They are then entitled to 10 weeks after the baby is born, even if the baby is born later then the expected date. Maybe this explains the frantic expressing? Funnily enough, midwives recommend you don’t go outside with the baby for at least one week. How old fashioned was my first thought, but upon reflection, how wonderful! There are so many pressures upon new mothers these days: to bounce back into shape, and ideally into those size 8 jeans you never fitted into in the first place, tidy home with of course Mary Berry style cakes for all visitors, and to be out and about with a perfect baby in the perfect pram! Although Dutch mothers are expected to go back to work after only 10 weeks and likely have some of the same pressures, that first week is really protected with being told that the baby should not go outside (which means mothers can stay in too). Furthermore, there is a kraamverzorgster helping several hours each day, and a midwife that comes round at least 4 times! I wonder if the care received in the first week has any impact on issues such as breastfeeding rates, bonding and postnatal depression, it would be interesting to even compare the UK with the Netherlands. PhD anyone?
Furthermore, there were other things that really struck a cord with me like continuity of care and the confidence of the midwives. The midwives are in a position to give great continuity of care, even in a small group practice, from beginning to end and make sure every midwife has seen the women so there is always a familiar face. Even I, in the short amount of time there met the same women and their families on several occasions, which was hugely satisfying all around! And yes we know that true continuity of care has better outcomes for women and their babies (Sandall et al., 2013) and is mentioned as a factor for work satisfaction for the midwives (Warmelink et al, 2015). However, for a lot of midwives in the UK to work this way would be utopia with the ever increasing work load and amount of women to see… it was so satisfying to see continuity of care as normal practise, not some dream… Of course the ability to work this way is also due to the clear separation of first and second line care as outlined by the Dutch Obstetric Indication List (aka the VIL). This list describes what is physiological and what should be considered a pathological pregnancy, labour and birth and decisions on whom to refer to second line and who to keep in first line care should be based on the VIL. Nevertheless, there is change happening in the Netherlands and midwives are fearful what this could mean for their autonomous independent practice serving pregnant women…
What is happening? Surprisingly and also controversially, findings from the Euro-Peristat (2008; 2013) showed the Netherlands to have one of the highest perinatal mortality rates in Europe in 1999 as well as in 2004. Unfortunately, the media seized this opportunity for scaremongering the general public that home births and midwives cause babies to die, and many unwarranted assumptions were made including that the separation of first and second line care is at fault (de Vries et al, 2013). It turned out that preterm births were included in these statistics and a reanalysis showed that the perinatal rate in the Netherlands is lower or not any different to other European countries, where first line care and high rates of homebirths are uncommon (de Jonge et al. 2013). Of course, these corrected findings were never reported in the media and the damage has been done. In view of the Euro-Peristat findings, the Dutch government is trying to ‘improve’ maternity care, depending what way you look at it, by creating more integrated care rather than a more specified divided first and second line care. This is how we work in the UK and there is a lot to be said to be able to provide care as a midwife for all women, no matter the perceived risks their pregnancy potentially carries.
In my short time spent with Chantal, Anke, Peggy, Carola and Rachelle I felt they were very certain of their care and decision-making. Listening to phone conversations with clients made me realise that they truly believed in the normality of pregnancy, labour and birth. Perhaps this sound funny but having spent the vast majority of my intrapartum training on an obstetric labour ward, I can vouch for how hard it is to keep hold of that belief and trust in a woman’s body! Regrettably with the current system in the UK, I think there are a lot of midwives have lost this belief and trust…. Notwithstanding the various years of experience of the Anno midwives, in my chats with them there was a positive self-assurance, even in the brand new midwife (she qualified only that week) whom I met when she came to help out one day, something I have not always felt chatting with (NHS) midwives in the UK. Absolutely, UK midwives also have self-confidence but it felt different … It could just be a cultural difference, with the Dutch being more extrovert by nature, or maybe it is because in the in the NHS, doctors are always in the background to keep a watchful eye out just in case resulting in midwives feeling and acting more cautious?
While a large proportion of midwives think integrated care can be a positive thing, there are many others who fear this change. Professor Raymond de Vries and his colleagues describe this glass half full or half empty standpoint poignantly in his article in Midwifery (2013). It gives the reader not only some ideas as to why the Dutch maternity care is changing but it also highlights the scary truth that scientific evidence is not enough to convince the greater public of the benefits of midwifery care, people also need to be convinced also on social and cultural levels (de Vries et al., 2013). I feel this is true not only for the Netherlands but also the UK and any other Western country where midwifery offers a safe and viable alternate option to obstetric care. Whatever direction integrated care will go in the Netherlands, I hope the Dutch people will keep their faith in their midwives and wish that the midwives I met and all their colleagues will keep believing in women, their bodies and stay positively self assured and confident in the care they provide! The Hague and the rest of the Netherlands are lucky to have them!
The Hague coastline
References:
Brouwers HA, Bruinse W, Dijs-Elsinga J, et al. (2014) Netherlands Perinatal Registry. Perinatal Care in the Netherlands 2013. Utrecht: Netherlands Perinatal Registry, 2014.
Birth Choice UK (2011). National Statistics. Available at http://www.birthchoiceuk.com/Professionals/BirthChoiceUKFrame.htm?http://www.birthchoiceuk.com/Professionals/statistics.htm.
De Vries, R., Nieuwenhuijze, M., Buitendijk, S., E. (2013). What does it take to have a strong and independent profession of midwifery? Lessons from the Netherlands. Midwifery, 29 (10), 1122-1128.
De Jonge, A,. Baron R., Westerneng, M., Twist, J,. Horton EK (2013) Perinatal mortality rate in the Netherlands compared to other European countries: a secondary analysis of Euro-PERISTAT data. Midwifery, 29 (8), 1011-1018.
Europeristat (2008,2013). Available at http://europeristat.com/. Last accessed 23 September 2015.
Sandall J., Soltani H., Gates S., Shennan A., Devane D. (2013) Midwife-led continuity models versus other models of care for childbearing women. Cochrane Database of Systematic Reviews, Issue 8. Art. No.: CD004667. DOI: 10.1002/14651858.CD004667.pub3.
Warmelink, C.,J., Hoijtink, K., Noppers, M., Wiegers, T., A., de Cock, P., Klomp, T., Hutton, E.,K. (2015). An explorative study of factors contributing to the job statisfaction of primary care midwives. Midwifery, 31 (4), 482-488.